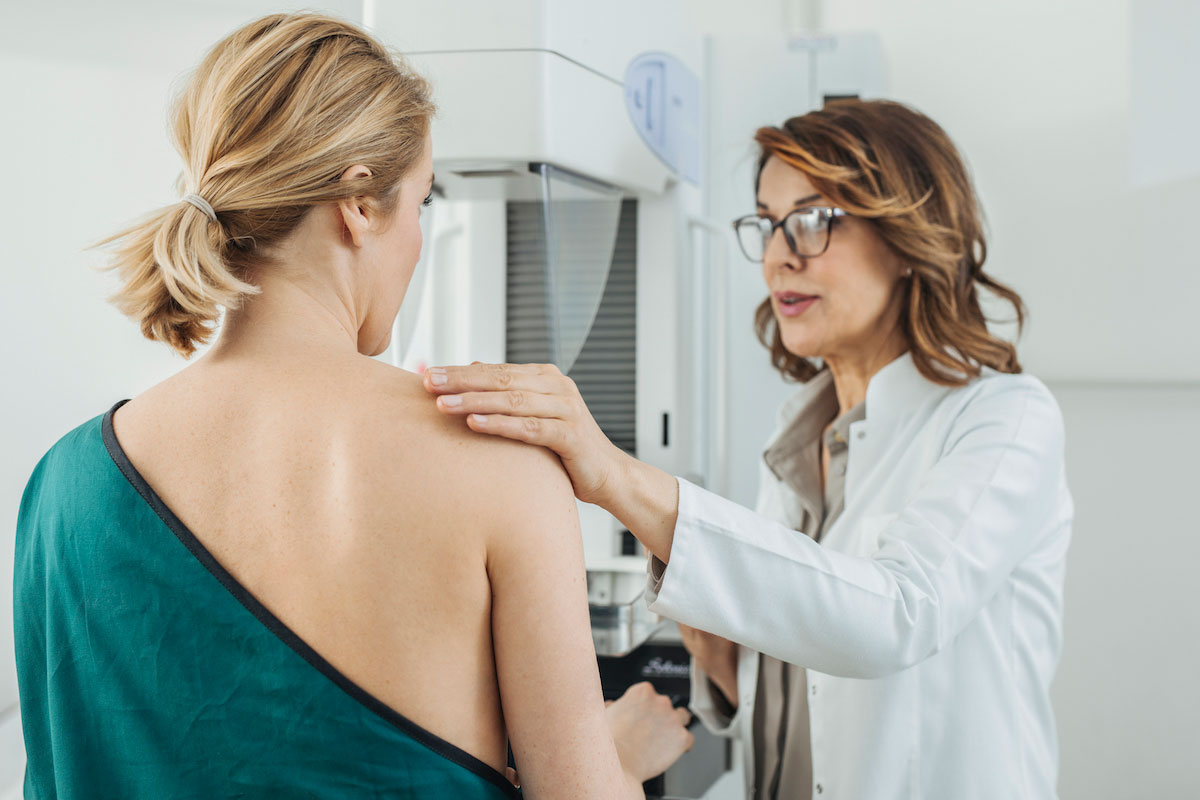
If age is just a number, why is the year a woman should start having annual mammograms so important – and so controversial?
Most recently, the American Society of Breast Surgeons (ASBrS) issued new guidelines advising women at average risk of breast cancer to begin annual mammograms at 40, which counters the American Cancer Society recommendation of 45 and a U.S. Preventive Services Task Force (USPSTF) advisory that moved the age from 40 to 50.
ASBrS members went further, too, urging that women be assessed for breast cancer risk at age 25 so they will better know when to start screening mammograms.
“It’s not uncommon for screening guidelines to change over time because they incorporate new knowledge gained through research and advances in technology. Mammograms are a prime example of this,” said Dr. Niamey P. Wilson, director of breast surgery, research and quality for the Hartford HealthCare Cancer Institute and breast surgery division lead for Hartford HealthCare Medical Group (HHCMG).
Noting that mammograms can detect cancer one to four years before a woman might feel a lump in her breast, Dr. Wilson said early detection means about a 20 percent reduction in death due to the disease. Moving the recommended age to 50 “maintains 80 percent of the benefit of this drop in mortality.”
Part of the reason for shifting the recommended start of annual mammography is cost, added Dr. Heather King, director of breast surgery at Hartford Hospital and breast division lead for HHCMG.
“The USPSTF released screening recommendations starting at age 50, instead of age 40, for mammograms for two reasons: screening at an early age leads to increased cost of medical care and anxiety in women with false positive results who might undergo breast biopsies that have benign findings,” Dr. King said. “The USPSTF guidelines are based on a mathematical risk calculation and do not focus on the women under 50 years old with a low or average risk of breast cancer.
“As a woman physician and mother in this age group, I would not rely on a mathematical calculation to determine my mortality. Life is precious and time spent making memories with our loved ones is priceless.”
Dr. Wilson agreed, saying, “While cost effectiveness is important in healthcare, I don’t think it’s the right thing to do for our patients to consider anything other than a recommendation that maintains 100 percent of the benefit. Women between the ages of 40 and 49 have a lower incidence of cancer compared to women 50 and older, but younger women tend to be diagnosed with more aggressive cancers – the cancers that would potentially be missed.”
The ASBrS recommendations “focus more on the lifespan of women,” Dr. King said.
This includes being informed and prepared as early as possible by undergoing risk assessment testing, which consists of a family history of breast cancer, especially at a young age; bilateral cancer; genetic mutations; and ovarian cancer. Dr. Kathleen Kurowski, medical director of breast surgery at Backus Hospital, said risk assessments – which can also address personal medical history, menstrual history, biopsy history and results, breast density, hormone therapy and genetic testing – stratify a woman’s individual risk for breast cancer.
“Assessing at 25 doesn’t mean you need mammograms at that age but if you wait until 40, you will miss some cancers,” she said. “Knowing that someone is high risk will allow screening to begin at an appropriate age. To discover someone carries a genetic mutation at the time of diagnosis of a late stage breast cancer could be considered a failure of screening.”
Besides earlier screening, women considered at high risk can also work with their provider on breast cancer prevention through lifestyle changes, medication or prophylactic surgery, she said.